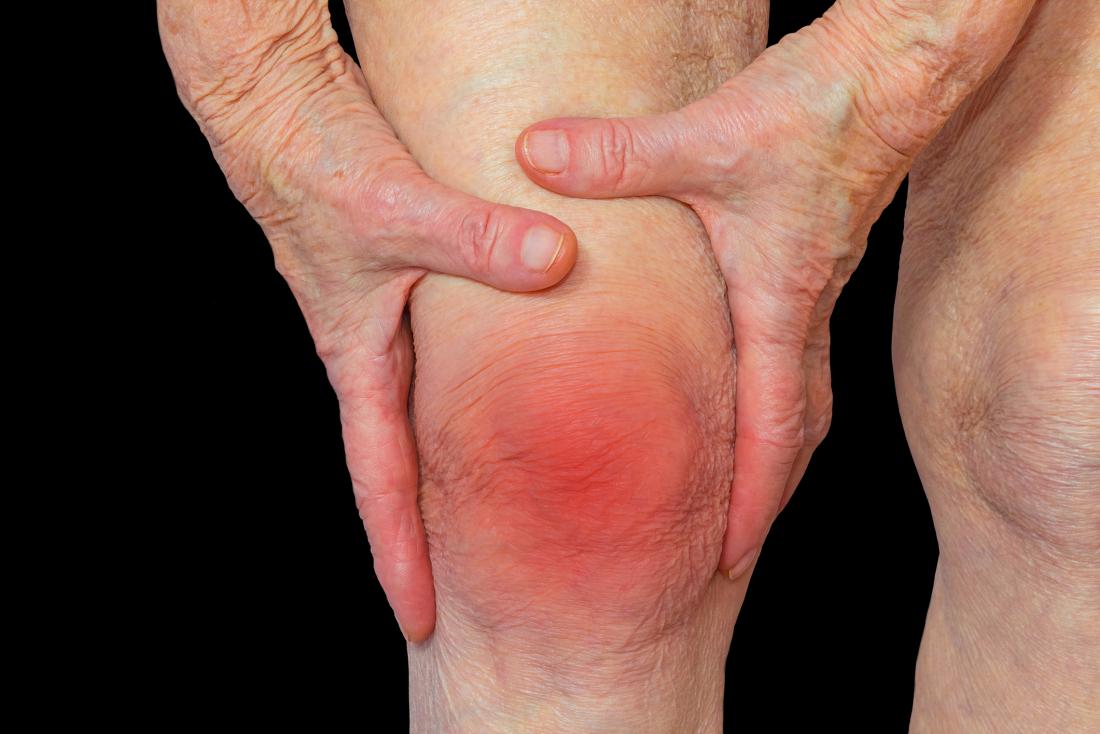
The ABCD’s of Arthritis
Arthritis affects millions of people all over the world. In fact, from the year 2010 – 2012, approximately 52.5 million adults (22.7%) in the United States were diagnosed with some form of arthritis. Unfortunately, this number is projected to reach 78 million (26%) by the year 2040. Aside from this, arthritis is also considered as one of the leading causes of disability attributed to work limitation and increased risk of falls and injuries (Centers for Disease Control and Prevention, 2016).
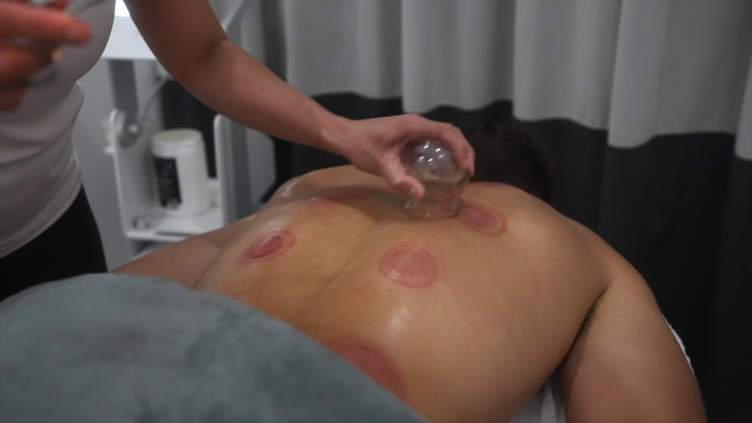
Though arthritis usually strikes during the peak of an individual’s most productive years of adulthood, there are several available approaches that can improve the quality of life despite being diagnosed with this disabling condition. This usually begins with our own initiative to increase awareness about the basics of arthritis, including its causes, symptoms and management. To help patients who are either at risk or currently suffering from this condition, this article focuses on the ABCDs of arthritis. Through this, they will be equipped with knowledge on how they can effectively deal with arthritis.
- ARTHRITIS
For people diagnosed with arthritis, pain is generally categorized as chronic that usually lasts for at least three months. Many patients describe this type of pain as aching, dull, burning or throbbing, which is comparable to a boa constrictor squeezing the affected joints. However, though arthritis can be well-managed by different treatment options, pain can also be sudden and unpredictable. This acute episode of pain and inflammation, referred to as arthritis flare, is oftentimes triggered by infection or stress. Though acute arthritic pain is only temporary, it can significantly affect our everyday life in terms of our capacity to perform daily tasks.
- BASIC TREATMENT.
One of the most common treatment options for arthritis is over-the-counter pain medication. However, this approach may not always address the problem effectively and may also pose certain risks. Hence, some patients skip the pills and prefer to try other alternative methods such as topical medications, exercise, physical therapy, meditation, acupuncture and heat or cold application.

- CRYOTHERAPY AS A REMEDY.
The benefits of cold therapy in relieving pain and inflammation secondary to arthritis have been recognized for thousands of years. In fact, in a study published in the Clinical and Experimental Rheumatology journal, it was revealed that both whole body and local cryotherapy significantly reduced the pain level perceived by patients with active rheumatoid arthritis (Hirvonen, Mikkelsson, Kautiainen, Pohjolainen, & Leirisalo-Repo, 2006). Moreover, different forms of cold therapy such as cold packs, ice massage, and cold baths are also known to reduce muscle spasm and inflammation in the acute stage (Krabak & Minkoff, 2012). Such benefit is said to be the impact of cryotherapy in lowering the temperature of the affected joint and in decreasing several mediators involved in joint inflammation and destruction (Guillot, et al., 2014).

- DOs AND DON’Ts FOR ARTHRITIS PAIN.
Though the above mentioned modalities can alleviate the pain and promote comfort, there are some other routines that patients can incorporate into their treatment plan. These methods may work wonders that can improve the quality of life and you’re the only one who can tell what best works for you. First, periods of activity must be balanced with periods of rest. Though pain can be disabling and may limit your activity, you must keep in mind that resting for long periods is counterproductive and may worsen the pain. Second, communicating with your family, friends and colleagues will help you deal with your obligations. This will let them know that there will be times that you will need extra help and some periods of rest to keep things running smoothly. Lastly, you may also try to practice relaxation techniques such as deep breathing exercises that can help minimize stress, a factor that can trigger episodes of arthritis flare.