Cryotherapy and Inflammation, Where is the Benefit and its Applications?
We probably all know the feeling, it hurts when you touch it, it feels swollen and warm, it looks red and you can actually feel your heart beat; the cardinal signs of an inflammatory response. This type of response might occur when you just sprained your ankle or recently had a surgery to your shoulder. When you think about it, you probably put ice on it or tried to cool it down in another way. It is commonly accepted that cryotherapy has an anti-inflammatory effect after soft tissue injury but why and how does it work?
Inflammation (from Latin inflammatio) is part of the complex biological response of body tissues to harmful stimuli, such as pathogens, damaged cells, or irritants, and is a protective response involving immune cells, blood vessels, and molecular mediators (Wikipedia). The function of inflammation is to eliminate the initial cause of cell injury, clear out necrotic cells and tissues damaged from the original insult and the inflammatory process, and initiate tissue repair.
The immediate phase after soft tissue injury is characterized by an acute inflammatory response. This often presents clinically with cardinal signs such as heat, redness, pain and swelling.
Inflammation can be classified as either acute or chronic. Acute inflammation is the initial response of the body to harmful stimuli and is achieved by the increased movement of plasma and white blood cells from the blood into the injured tissues. Chronic inflammation leads to a progressive shift in the type of cells present at the site of inflammation and is characterized by simultaneous destruction and healing of the tissue from the inflammatory process.
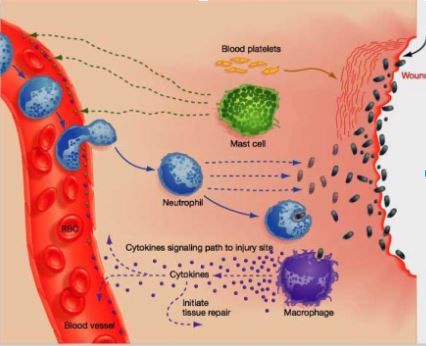
In short the inflammatory response consist of 6 steps (see illustration 1):
- After signaling, mast cells secrete factors that mediate vasodilation and vascular constriction
- Delivery of blood, plasma, and cells to the injured area increases
- Neutrophils secrete factors that kill and degrade pathogens
- Neutrophils and macrophages remove pathogens by phagocytosis
- Macrophages secrete cytokines that attract immune system cells to the site and activate cells involved in tissue repair
- Inflammatory response continues until the foreign material is eliminated.
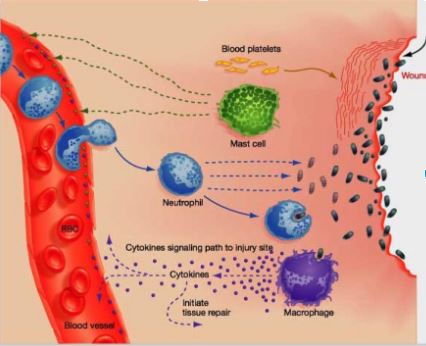
Illustration 1: schematic representation of the inflammatory response in relation to a wound. The different steps also account for different types of soft tissue injuries
The applications of cryotherapy can differ from using an ice bag, the use of cold water, applying localized cold air or the exposure to whole body cryotherapy. In general, cryotherapy decreases the temperature of the skin and muscle, which reduces blood flow and metabolism, which results in a decrease in inflammation. More specifically, cryotherapy might have an effect on a reduction of secondary cell injury, guide the release of white blood cells, reduce the incidence of apoptosis and reduce the blood flow and edema formation. These effects are well summarized and appraised according to the current literature by Bleakly & Davidson (2010).
Merrick et al. (1999) was among the first to experimentally show that prolonged cooling (5 hours!) retarded the secondary injury in the acute treatment after a crush injury. And Schaser et al. (2007) is actually one of the few clinical studies that focused on measuring the potential difference in the inflammatory response after a soft tissue injury. They concluded that prolonged cooling did reduce inflammation. Westermann et al. (1999) found that the number of apoptotic cells was significantly higher in untreated control when compared to the cryotherapy group. There seems to be a relative balance between the need for inflammation to stimulate repair and the need to limit inflammation because of the additional damage it causes. This potential damage is caused by the activation of white blood cells (respiratory burst) which in the case of overproduction may cause collateral damage. This is especially unwanted in the case of a close soft tissue injury (ankle sprain) with no association with bacteria or infection. According to Butterfield et al. (2006) elucidating this balance should be the key goal of current inflammation research. Although more research is needed, it seems clear that cryotherapy has a potential role in reducing the inflammatory response.
Some basic guidelines for targeting the inflammation in soft tissue injury;
- Local cryotherapy should be applied prolonged (it is essential to decrease the intra-articular temperature) and multiple times in the acute phase of a soft tissue injury to have an direct effect on inflammatory response.
- After the acute phase of the injury (48-72 hours), the focus of using cryotherapy should shift towards the presented symptoms mainly by guiding pain. In this phase one can think of different types of cryotherapy.
References
- Bleakley, C. M. & Davison, G. W. Cryotherapy and inflammation: evidence beyond the cardinal signs. Physical Therapy Reviews 15, 430–435 (2010).
- Butterfield, T. A., Best, T. M. & Merrick, M. A. The dual roles of neutrophils and macrophages in inflammation: a critical balance between tissue damage and repair. J Athl Train 41, 457–465 (2006).
- Merrick, M. A., Rankin, J. M., Andres, F. A. & Hinman, C. L. A preliminary examination of cryotherapy and secondary injury in skeletal muscle. Med Sci Sports Exerc 31, 1516–1521 (1999).
- Schaser, K.-D. et al. Prolonged superficial local cryotherapy attenuates microcirculatory impairment, regional inflammation, and muscle necrosis after closed soft tissue injury in rats. Am J Sports Med 35, 93–102 (2007).
- Westermann, S., Vollmar, B., Thorlacius, H. & Menger, M. D. Surface cooling inhibits tumor necrosis factor-alpha-induced microvascular perfusion failure, leukocyte adhesion, and apoptosis in the striated muscle. Surgery 126, 881–889 (1999).
- https://en.wikipedia.org/wiki/Inflammation